What Causes Low Neutrophil Count (Neutropenia) and How Is It Treated?
Neutropenia is a medical condition characterized by an abnormally low number of neutrophils in the blood. Neutrophils are a type of white blood cell that play a crucial role in the body’s immune defense against bacterial and fungal infections. When the neutrophil count falls below normal levels, the body becomes more vulnerable to infections. Neutropenia is an important topic in biology and medicine, especially for NEET aspirants, as it is closely related to immunity, hematology, and disease mechanisms.
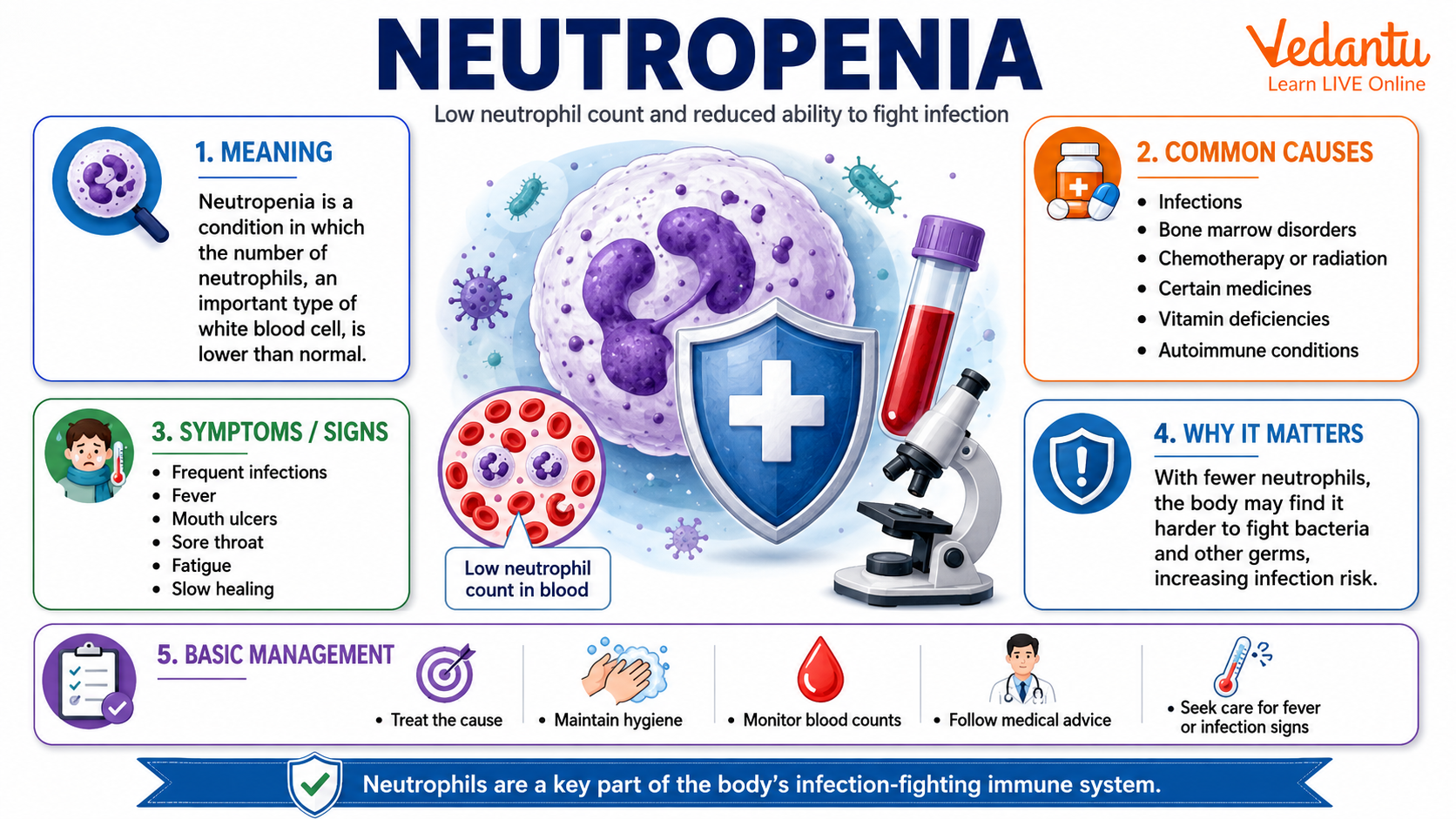
What is Neutropenia?
Neutropenia refers to a decrease in the absolute neutrophil count (ANC) in peripheral blood. In healthy individuals, neutrophils form about 50 to 70 percent of total white blood cells. They are the first responders to microbial infection and help destroy pathogens through phagocytosis and enzyme release.
Neutropenia is generally diagnosed when the absolute neutrophil count falls below 1500 cells per microliter of blood. The severity of neutropenia determines the risk of infection.
Classification of Neutropenia Based on ANC
| Severity | Absolute Neutrophil Count (cells per microliter) | Risk of Infection |
|---|---|---|
| Mild | 1000 to 1500 | Low risk |
| Moderate | 500 to 1000 | Moderate risk |
| Severe | Less than 500 | High risk and life threatening |
As the neutrophil count decreases, the ability of the body to fight infections significantly reduces. Severe neutropenia requires urgent medical attention.
Causes of Neutropenia
Neutropenia can occur due to decreased production of neutrophils, increased destruction, or abnormal distribution in the body. The causes can be broadly classified as follows:
1. Decreased Production in Bone Marrow
- Aplastic anemia
- Leukemia and other bone marrow cancers
- Chemotherapy and radiotherapy
- Vitamin B12 or folate deficiency
2. Increased Destruction
- Autoimmune disorders such as lupus
- Severe bacterial infections
- Drug induced immune reactions
3. Congenital Causes
- Severe congenital neutropenia
- Cyclic neutropenia
Signs and Symptoms
Neutropenia itself may not cause direct symptoms, but it increases susceptibility to infections. Common clinical features include:
- Fever, often the first and only sign
- Recurrent bacterial infections
- Mouth ulcers and sore throat
- Skin abscesses
- Pneumonia or urinary tract infections
In severe cases, even minor infections can rapidly become systemic and life threatening.
Diagnosis of Neutropenia
The diagnosis of neutropenia is primarily made through laboratory investigations. A complete blood count test is the most important diagnostic tool.
- Complete Blood Count to measure total white blood cells and absolute neutrophil count
- Peripheral blood smear to examine cell morphology
- Bone marrow examination if production defect is suspected
- Vitamin level testing or autoimmune screening if required
Treatment and Management
Treatment depends on the severity and underlying cause of neutropenia. The primary goal is to prevent infections and correct the root cause.
- Administration of antibiotics in case of infection
- Granulocyte colony stimulating factor to stimulate neutrophil production
- Discontinuation of causative drugs
- Bone marrow transplant in severe congenital cases
- Protective isolation in severe neutropenia
Prevention and Precautions
Patients with neutropenia should take special precautions to minimize infection risk.
- Maintain proper hand hygiene
- Avoid crowded places during severe neutropenia
- Consume well cooked and hygienic food
- Regular medical follow up and blood tests
Importance of Neutropenia for NEET
Neutropenia is frequently linked to questions from the chapters on Human Physiology and Human Health and Disease. NEET aspirants should understand the role of neutrophils in innate immunity, the concept of absolute neutrophil count, and the clinical significance of low white blood cell counts. Questions may be conceptual, clinical based, or related to immune response mechanisms.
Key Points to Remember
- Neutropenia is defined as ANC less than 1500 cells per microliter
- Severe neutropenia increases risk of life threatening infections
- It may result from decreased production, increased destruction, or congenital defects
- Complete blood count is essential for diagnosis
- Granulocyte colony stimulating factor is commonly used in treatment
In summary, neutropenia is a significant hematological condition that reflects impaired immune defense. A clear understanding of its causes, classification, symptoms, and management is essential for medical entrance examinations and for building strong conceptual knowledge in human physiology and pathology.
FAQs on Neutropenia: Understanding Low Neutrophil Levels
1. What is Neutropenia?
Neutropenia is a medical condition characterized by an abnormally low level of neutrophils, a type of white blood cell essential for fighting infections.
• Neutrophils are part of the immune system and help destroy bacteria and fungi.
• It is diagnosed when the Absolute Neutrophil Count (ANC) falls below 1,500 cells per microliter.
• Severe neutropenia occurs when ANC is below 500.
• Commonly associated terms: low white blood cell count, immune deficiency, bone marrow disorder.
2. What are the main causes of Neutropenia?
Neutropenia can result from decreased production or increased destruction of neutrophils in the body.
• Bone marrow disorders like leukemia or aplastic anemia
• Chemotherapy and radiation therapy
• Severe bacterial or viral infections
• Autoimmune diseases such as lupus
• Nutritional deficiencies (Vitamin B12 or folate)
• Certain medications including antibiotics and antithyroid drugs
3. What are the common symptoms of Neutropenia?
Neutropenia itself may not cause symptoms, but it increases the risk of frequent and severe infections.
• Recurrent fever (often the first sign)
• Mouth ulcers and sore throat
• Skin infections or abscesses
• Pneumonia or respiratory infections
• Pain during urination due to urinary tract infection
People often ask: Does neutropenia cause fever? Yes, fever is a key warning sign.
4. How is Neutropenia diagnosed?
Neutropenia is diagnosed through a blood test that measures the Absolute Neutrophil Count (ANC).
• Complete Blood Count (CBC) test
• Calculation of ANC from white blood cell count
• Bone marrow biopsy in severe or unexplained cases
• Additional tests to identify infections or autoimmune causes
This condition is commonly detected during routine blood investigations.
5. What are the types of Neutropenia?
Neutropenia is classified based on severity and duration.
• Mild Neutropenia: ANC 1,000–1,500
• Moderate Neutropenia: ANC 500–1,000
• Severe Neutropenia: ANC below 500
• Acute Neutropenia: Develops rapidly
• Chronic Neutropenia: Lasts more than three months
These classifications help determine infection risk and treatment approach.
6. How is Neutropenia treated?
Treatment of neutropenia depends on its underlying cause and severity.
• Antibiotics to treat or prevent infections
• Granulocyte Colony-Stimulating Factor (G-CSF) to boost neutrophil production
• Stopping or adjusting causative medications
• Bone marrow transplant in severe cases
• Nutritional supplementation if due to deficiency
People also search: Can neutropenia be cured? It can be managed effectively with proper treatment.
7. Who is at risk of developing Neutropenia?
Certain groups are more vulnerable to developing neutropenia due to medical treatments or underlying diseases.
• Cancer patients undergoing chemotherapy
• Individuals with autoimmune disorders
• Patients with bone marrow diseases
• People with severe infections
• Individuals with genetic conditions like congenital neutropenia
Understanding risk factors helps in early detection and prevention.
8. What complications can arise from Neutropenia?
The most serious complication of neutropenia is life-threatening infection.
• Sepsis (blood infection)
• Pneumonia
• Skin and soft tissue infections
• Delayed wound healing
• Febrile neutropenia, a medical emergency
Without adequate neutrophils, the immune system cannot effectively fight pathogens.
9. What is Febrile Neutropenia?
Febrile neutropenia is a dangerous condition where a person with neutropenia develops a high fever indicating possible infection.
• Defined as fever above 38°C (100.4°F) with low ANC
• Common in cancer patients receiving chemotherapy
• Requires immediate hospitalization
• Treated with broad-spectrum intravenous antibiotics
It is considered a medical emergency due to high infection risk.
10. Can Neutropenia be prevented?
Neutropenia cannot always be prevented, but infection risk can be reduced with proper precautions.
• Maintain good personal hygiene
• Avoid crowded places during low immunity
• Eat well-cooked and hygienic food
• Regular monitoring of white blood cell count
• Prophylactic medications in high-risk patients
Preventive care is especially important for individuals undergoing chemotherapy or immunosuppressive therapy.